 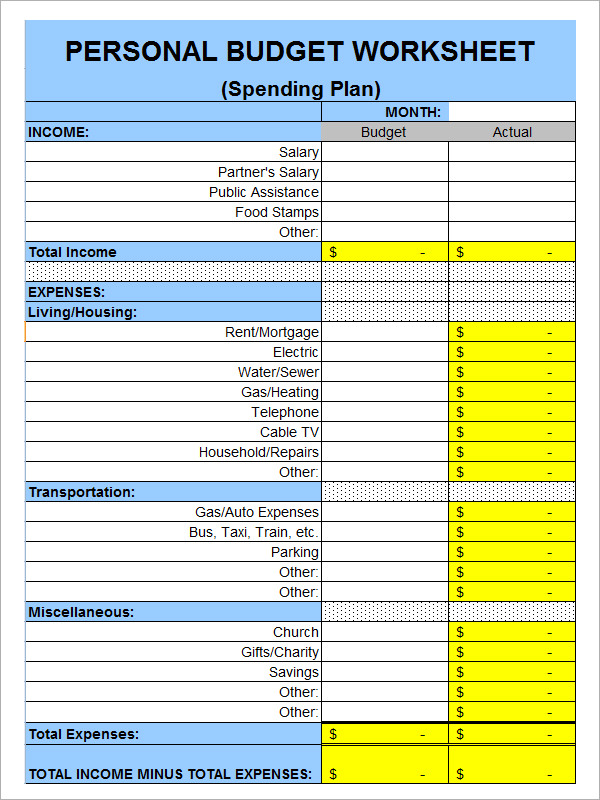 
The interaction of these elements to produce value-based health care is illustrated in Figure 1. Policy makers and payers contribute to the value equation by designing health policies and benefit packages that promote beneficiaries' access to and use of timely, appropriate health care services. Cost-effectiveness is achieved, in the short term, through financial penalties for poor provider performance and, in the long term, through a reduced need for more complex and expensive services resulting from unattended diseases and disorders. 11 Provider accountability is achieved through the implementation of evidence-based practice standards, directed toward the reduction of unwarranted variation, against which performance is measured. Value-based health care aims to improve access to quality services and lower cost while requiring greater accountability on the part of all stakeholders within the health care system. 10 Although elements of this legislation continue to be debated, the commitment to value-based health care services already was well-established among policy makers, regulators, third-party payers, and some consumers. This paradox of high costs, variable quality, and inconsistent access to services in the face of overwhelming demand was central to the health care reform deliberations that resulted in passage of the Patient Protection and Affordable Care Act (PL 111-148) in 2010. 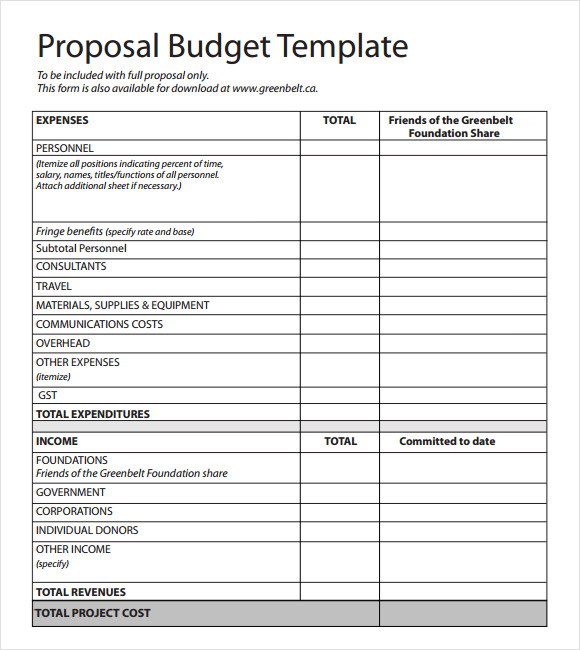
Approximately 40% of this cohort is estimated to have a disability and is in need of health care services. By 2030, individuals aged 65 years and older will account for almost 20% of the total US population. 8 Inadequate access is particularly troubling given the projected need for services. Furthermore, 1 in 5 Americans experience delays in or denials of needed health care. 7 In 2010, the Agency for Healthcare Research and Quality (AHRQ) reported that racial and ethnic minorities and individuals with lower socioeconomic status often receive poorer quality of care and have greater difficulty accessing care compared with individuals who are white or who earn higher incomes. Sociodemographic disparities and inadequate access to needed services for many individuals are compounded by the high cost and variable quality of health care. 3 This report, along with other health policy studies, 4– 6 indicated a high variability in health care delivery across the nation. The Institute of Medicine (IOM) noted that rapid technological expansion and subsequent complexity resulted in safety failures and suboptimal benefits. 2 Concern about financial sustainability is magnified by the recognition that increased health care spending does not fully address the needs of Americans or result in higher-quality care or greater patient satisfaction with the delivery system. 1 Long-term performance of the health care delivery system is widely viewed to be unsustainable economically. 1 Furthermore, expenditures are projected to grow an average of 6.1% per year from 2009 to 2019. In 2009, the United States spent more than $2.5 trillion, or 17.6% of its gross domestic product, on health care. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
